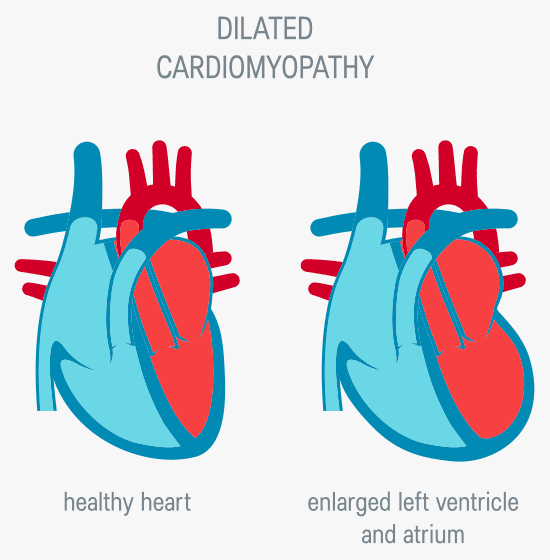
What is Peripartum Cardiomyopathy?
Peripartum Cardiomyopathy (PPCM) is a form of heart failure during the systolic phase of pumping i.e. the heart pumping with force to circulate blood in the body.
PPCM typically presents at late-stages pregnancy and in the early post-partum (after birth) period, if there are no other causes for heart failure found.
When experiencing PPCM, your left ventricle on your heart (which is responsible for pumping blood into your body) can become enlarged and weakened, therefore not pumping blood properly around the body.
As a result, blood can build up in areas of the body such as the lungs, leading to less oxygen for you and can have a noticeable effect such as breathlessness and extreme fatigue.
There are no clear underlying reasons why you may have developed PPCM, however there are suggestions from research that pregnancy-specific related conditions such as pre-eclampsia as well as risk factors such as diabetes and obesity are linked to PPCM. See the risk factors for PPCM section.

Statistics
Most data comes from the United States, where it is estimated that PPCM exists somewhere between one in 900 to one in 4000 births.
It is estimated that 50% of women who have PPCM had pre-eclampsia during their pregnancy, however, this information is still being researched.
It is estimated that around 50-80% of women with PPCM will recover within the first six months of diagnosis, a figure which has improved substantially due to better recognition and treatment of PPCM.
Signs & symptoms of Peripartum Cardiomyopathy
It can be difficult to diagnose PPCM and typically it is a delayed diagnosis as many of the signs and symptoms are similar to that of normal changes to your body during pregnancy.
It is worth remembering that most women who have PPCM will develop the signs and symptoms within the first few months after giving birth.
Here are the signs and symptoms of PPCM:
- Shortness of breath
- Fluid retention and swelling around the legs
- Palpitations
- Fatigue
- Chest pain
- Abdominal discomfort due to swelling of the liver
- Low blood pressure (hypotension)
Risk Factors of Peripartum Cardiomyopathy
There are a number of risk factors which have been associated with PPCM, however it is still not yet clear how women contract PPCM.
Below are some suggested risk factors for PPCM:
- History of high blood pressure (hypertension)
- Older age in pregnancy
- Family history of cardiomyopathy
- Had previous pregnancies
- Overweight
- Ethnicity (African-American women account for 40% of cases in the United States)
- Preeclampsia in pregnancy. Information on pre-eclampsia can be found here.
Treatment for Peripartum Cardiomyopathy
Treatment for PPCM is similar to the management of heart failure; below is a list of ways your doctor could help you manage your PPCM.
- Fluid restriction: In order to reduce the pressure on your heart, your doctors may recommend only drinking between 1.5-2L of fluid daily.
- Reduce salt intake: Aim for less than 2g per day. This page from the Queensland Government has some tips and tricks for reducing your salt intake.
- Hospital admission: Having a stay in hospital may be required to get your symptoms under control.
- Investigations: You may need some investigations conducted to determine your severity of PPCM. These include blood tests, ultrasounds (echo) of the heart as well as a chest x-ray.
- Medications: Medications may be prescribed to you to improve your symptoms and heart function. These medications include diuretics to help reduce fluid levels, beta blockers to relax your heart rate and ACE inhibitors to help your blood pressure. We recommend you discuss these with your doctor and pharmacist.
What you need to know
Further information
Useful links